During ablations and electrophysiology studies, the surgeon must have a clear idea about where scars and other relevant items are within the heart. Normally, this information is displayed on a computer monitor and the doctors use mouse or joystick to zoom, rotate or slice the images. However, during these procedures the surgeon needs to look away from the patient, which creates problems with maintenance and sterility.
Scientists at the Beth Israel Deaconess Medical Center (BIDMC) in Boston have found a novel way to solve this problem. They’ve tested the use of Augmented Reality (AR) to help them visualize myocardial scarring in the heart as they perform ventricular tachycardia ablation or other electrophysiological interventions, reports BIDMC.
Augmented reality is a technology that augments or superimposes computer-generated information on a user’s view of the real world. Researchers believe AR can help doctors better visualize complex medical data, particularly before and during medical procedures, enabling them to interactively explore data in three dimensions.
Jihye Jang, a PhD Candidate at the Cardiac Magnetic Resonance (MR) Center at BIDMC, and colleagues assessed AR’s potential to help cardiologists visualize myocardial scarring in the heart as they perform ventricular tachycardia ablation or other electrophysiological interventions.

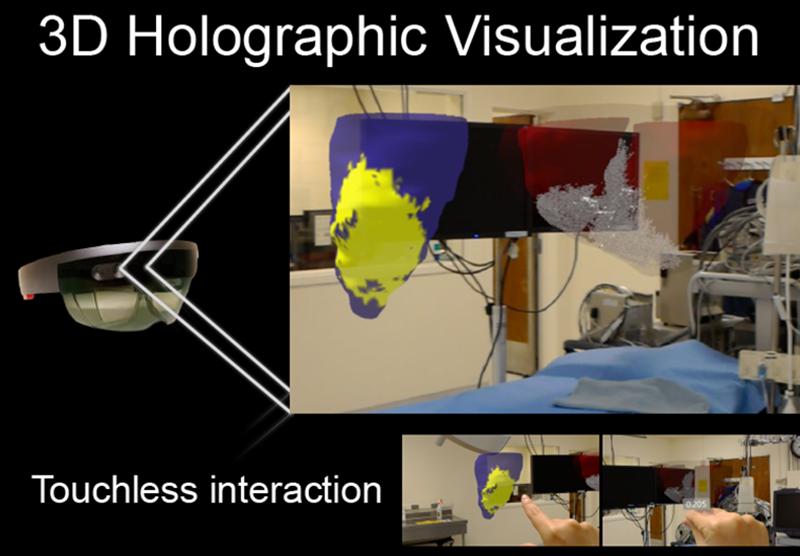
“Augmented reality allows physicians to superimpose images, such as MRI or CT scans, as a guide during therapeutic intervention,” said Jang. “Our report shows exciting potential that having this complex 3D scar information through augmented reality during the intervention may help guide treatment and ultimately improve patient care. Physicians can now use AR to view 3D cardiac MR information with a touchless interaction in sterile environment.”
In a study with animals that were induced to suffer heart attacks, the researchers applied the AR technique as they generated holographic 3D scar in five animal models that underwent controlled infarction and electrophysiological study. An operator and mapping specialist viewed the holographic 3D scar during electrophysiological study.
Related FundamentalVR Tool Combines VR with Haptic Sensors to Make VR Surgery Feel Like Real Thing
The clinicians that performed the procedures found the technique useful to have scar information during the intervention.
“Our report is one of the first efforts to test augmented reality in cardiovascular electrophysiological intervention,” said Jang. “Our next steps will expand the use of AR into treatments for arrhythmia by merging the scar information with electrophysiology data.”