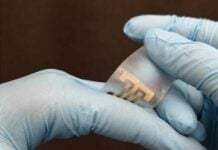
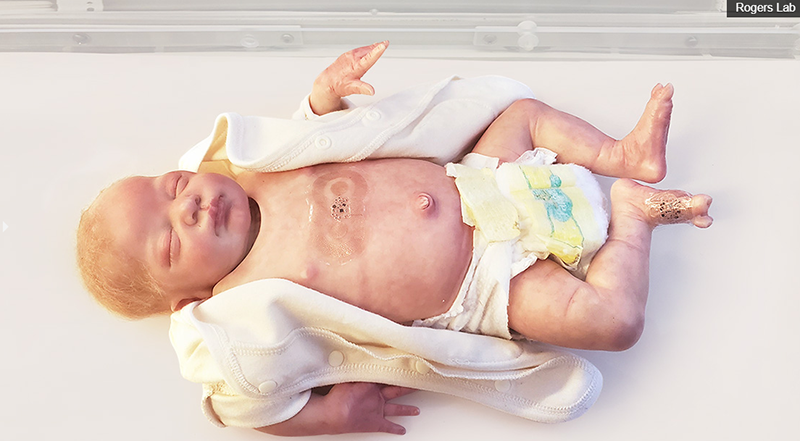
For parents, it’s heartbreaking to see their prematurely born baby in the neonatal intensive care unit (NICU) with wires and sensors sticking out of their bodies, posing a barrier to parent-baby cuddling and physical bonding. During these times, babies, as much as parents, need physical and emotional bonding badly. Northwestern University researchers have now developed a pair of soft, flexible wireless body sensors that may soon replace the tangle of wire-based sensors that are currently used in hospitals’ NICU.
Related Special Pacifier Plays Songs to help Premature Babies Develop Skills to Suck for Milk
A series of human studies on the device were conducted by researchers at Prentice Women’s Hospital and the Ann & Robert H. Lurie Children’s Hospital in Chicago. The results showed that the data delivered by the wireless sensors were as precise and accurate as that of data derived from traditional monitoring systems. The wireless patches also are gentler on a newborn’s fragile skin and allow for more skin-to-skin contact with the parent, reports Northwestern Now.
The study was published in the journal Science.
The benefits of the new sensors go beyond its lack of wires – measuring more than what’s possible with today’s clinical standards.
From opposite ends of the body, the dual wireless sensors monitor babies’ vital signs such as heart rate, respiration rate and body temperature. One sensor lies across the baby’s chest or back, while the other wraps around a foot. (The chest sensor measures 5 centimeters by 2.5 centimeters; the foot sensor is 2.5 centimeters by 2 centimeters). This strategy allows physicians to gather an infant’s core temperature as well as body temperature from a peripheral region.
Both sensors are very light and each weigh as much as a raindrop.

“Differences in temperature between the foot and the chest have great clinical importance in determining blood flow and cardiac function,” says John A. Rogers, a bioelectronics pioneer, who led the technology development. “That’s something that’s not commonly done today.”
The wireless sensor communicates through a transmitter placed underneath the crib’s mattress. The antenna transmits data to displays at the nurses’ station. Although it can be sterilized and reused, the sensor is cheap enough (about $10) that it can simply be discarded after 24 hours and replaced with a new one to eliminate any risk of infection.
Related Masimo’s Rainbow Acoustic Monitoring RAS-45 Breathing Sensor for Babies Gets FDA Clearance
When will the New Device Be Available in Hospital?
Rogers estimates that his wireless sensors will appear in U.S. hospitals within the next two to three years. With support from two major nonprofit organizations, Rogers’ team expects to send sensors to tens of thousands of families in developing countries over the next year as part of an international effort, said the Northwestern Now report.
“We’re proud of the fact that this technology isn’t just limited to advanced NICUs in developed countries,” says, Dr. Shuai (Steve) Xu, a co-author of the study. “The technology can be adapted with minimal modification for low-resource settings.”